An Evidence-Based Biased Opinion by Eisen Liang
Hysterectomy is a major surgical operation that requires general anaesthetic, a few days in the hospital and 4-6 weeks of downtime to recover. While the procedure is successfully used to treat some serious conditions, it is worth knowing the possible side effects of hysterectomy.
In this article, we will uncover the most common hysterectomy risks and long-term side effects. Also, we will find out if a hysterectomy is the only solution in the 21st Century and what other options might be available.
Table of Contents
The Most Common Side Effects of Hysterectomy
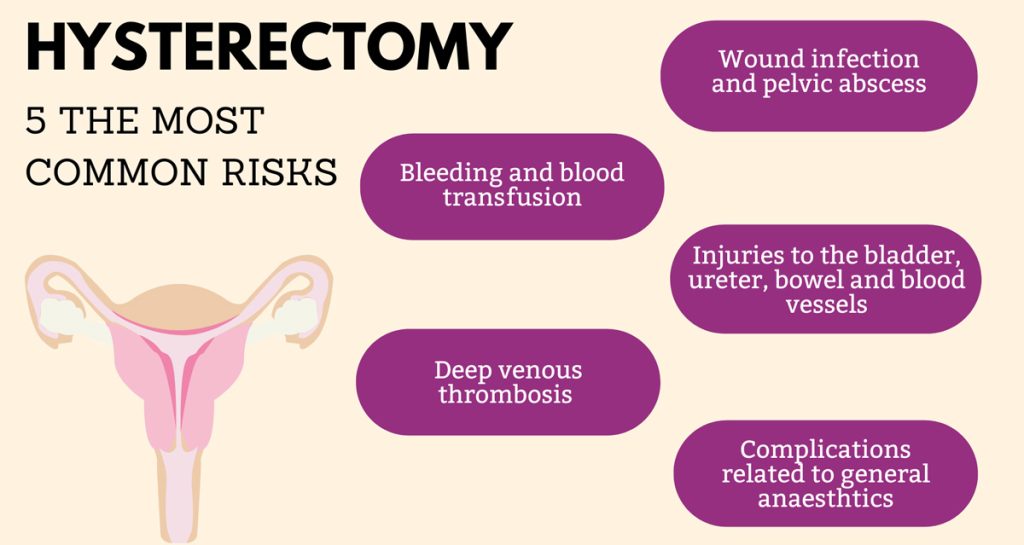
Since a hysterectomy is a major surgical operation, it comes with the same risks as any other major surgery. This can include:
-
-
- Wound infection and pelvic abscess
- Bleeding and blood transfusion
- Deep venous thrombosis (DVT)
- Injuries to other organs such as bladder, ureter (the tube connecting kidney to bladder), bowel and blood vessels
- Complications related to general anaesthetics
-
Although rare, some of the most severe complications associated with hysterectomies are injuries to:
-
-
- Bladder
- Ureter (the tube connecting kidney to bladder)
- Bowel
- Blood vessels
-
Suffering one of these complications means you will have to go to the theatre a second time for repairs by another specialist.
Even with modern surgical methods, the risk of severe complications from hysterectomy remains at a high rate of 3.5 to 11.0%.
Studies from Melbourne reported a hysterectomy mortality rate of 1.5 /1,000 in Australia2.
Vaginal, laparoscopic or robotic hysterectomy might reduce recovery time but might not reduce the risk of hysterectomies.
Long Term Side Effects of Hysterectomy
Early menopause
Women who had a hysterectomy may enter menopause almost four years earlier 3. Blood supply to the ovary may be compromised during surgery by ligation, spasm or thrombosis.
Pelvic floor prolapse and urinary incontinence
These might occur many years after hysterectomy4. Hysterectomy removes supporting structures and weakens the pelvic floor. Removal of or cutting of the ligaments supporting the cervix and vagina may predispose to the development of prolapse. Furthermore, the effectiveness of prolapse repair can be compromised by removing the cervix and ligaments, which are used to anchor an effective repair.
Sexual dysfunction
The effect of a hysterectomy on a woman’s sex life depends on the individual. Women need to know that after a hysterectomy, especially a total hysterectomy5, they may have less libido and less intense orgasms. This can happen when nerves are damaged, the anatomy of the vaginal area changes, or when the uterus stops contracting. This can make it hard or impossible to have an orgasm, or it can change how it feels. Those women whose sex lives are affected by their severe menstrual symptoms may find that hysterectomy improves sex life afterward.
Constipation
Some women may experience constipation after a hysterectomy due to nerve damage6.
Post Hysterectomy Syndrome
Women who have had a hysterectomy take longer to recover than those who have undergone other major surgery. Symptoms include urinary problems, tiredness, and depression. The root cause is unknown, and the condition has been called Post Hysterectomy Syndrome7. It is commonly believed that this problem occurs due to a hormone imbalance after having a hysterectomy.
Coronary heart disease
A recently released study8 discovered a 33% increased risk of coronary heart disease in women who have had a hysterectomy, even if their ovaries are not removed. If a hysterectomy is performed on women younger than 35, that number jumps to 250%.
Is Hysterectomy Still the Only Solution in the 21st Century?

Australia tops the OECD in doing hysterectomy to women
If diagnosed with uterine cancer, there is no doubt hysterectomy would be absolutely necessary. However, in a developed country like Australia, most hysterectomies are performed for benign conditions like fibroids or adenomyosis. It is estimated that 30 000 hysterectomies are done in Australia each year.
There is a non-surgical procedure performed by radiologist called uterine fibroid embolisation (UFE)/ uterine artery embolisation (UAE), that has proven effective for most women suffering from symptoms related to fibroids or adenomyosis.
UFE/UAE provides an alternative to hysterectomy for women with fibroids and adenomyosis, allowing them to keep their uterus, potentially preserving fertility, and avoid the risks and long recovery times associated with major surgery.
Final Thought
Hysterectomy is a major surgery that usually requires a long road to recovery. In many cases should be considered a last resort. Before going through this procedure, patients should be sure they have explored all other options, and consider the side effects of hysterectomy. As always, you should feel comfortable talking to your doctor to discuss whether a hysterectomy is right for you and consider alternative treatments like UFE and UAE.
Read more about UAE as an effective non-surgical alternative to hysterectomy HERE
You can also read about UFE as an effective treatment for fibroids HERE
References:
-
-
- Update 2019 : Differentiating uterine leiomyomas (fibroids) from uterine sarcomas Elizabeth A Stewart, MD https://www.uptodate.com/contents/uterine-fibroids-leiomyomas-differentiating-fibroids-from-uterine-sarcomas Accessed 28th August 2019
- Ten-year review of hysterectomy morbidity and mortality: can we change direction? Varol, N; Healey, M; Tang, P; Sheehan, P; Maher, P; Hill, D Australian & New Zealand Journal of Obstetrics & Gynaecology, 2001 Aug, Vol.41(3), pp.295-302
- The association of hysterectomy and menopause: a prospective cohort study. Farquhar CM, Sadler L, Harvey SA, Stewart AW. BJOG: An International Journal of Obstetrics & Gynaecology. 2005;112(7):956–962.
- Urinary Symptoms following hysterectomy Smith P, Roberts M, Slade N. British Journal of Urology. 1970;42(1):3–9.
- Supra Vaginal Uterine Amputation VS. Hysterectomy: Effects on libido and orgasm. Kilkku P, Grönroos M, Hirvonen T, Rauramo L. Acta Obstetrica et Gynecologica Scandinavica. 1983;62(2):147–152.
- Papachrysostomou M. Disordered colorectal motility in intractable constipation following hysterectomy. Smith A, Varma J, Binnie N, British journal of surgery. 1990;77(12):1361–1365.
- A post-hysterectomy syndrome. Richards D. The Lancet. 1974;304(7887):983–985.
- Cardiovascular and metabolic morbidity after hysterectomy with ovarian conservation: a cohort study Laughlin-Tommaso, K., Shannon; Khan, L., Zaraq; Weaver, Y., Amy ; Smith, A., Carin ; Rocca, A., Walter ; Stewart, A., Elizabeth Menopause, 2018, Vol.25(5), p.483-492
- https://www.nhs.uk/conditions/hysterectomy/risks/
-

