If it took 15 years for an intelligent executive in a pharmaceutical company to sort out her heavy menstrual bleeding, something is not right in our medical care for women.
When conservative treatments failed, women were forced to choose between hysterectomy or putting up with debilitating symptoms.
KLB is a 40 year old Pharmaceutical executive, mother of 4 children age 5-23. Here is her journey to search for diagnosis and effective treatment of her menstrual issues.
For more than 15 years I’ve been suffering with heavy periods, my heavy periods caused me to have low iron which caused a number of other issues. I have seen numerous doctors during this time, specialists, GPs and even homeopaths trying to understand why my period was causing such disruption to my life.I wasn’t really aware that my normal was in fact not the “average normal period” until a discussion with my friend in my late 20’s.
For me bleeding through a super tampon and super pads together and then my clothes was a normal period. I can recall a number of situations when I had to leave work due to excessive bleeding and have used so many sick days during my heavy days of my period because I literally felt I couldn’t leave the house without severe embarrassment.
For my husband and family they had to schedule activities around my period, I wouldn’t be able to take my kids to weekend activities due to the excessive bleeding. During my period it was not unusual to wake 3 or more times a night to change my pad and I had purchased a waterproof mattress protector to utilise during my period. I was tired, grumpy and hyper emotional during the period. I sat on a towel on the couch to try and minimise the risk of staining.
For me the pain was another issue. I regularly had to take prescription pain killers to deal with the pain.
My menstrual issue has controlled my life for such a long time I had developed a number of strategies to try and reduce possible embarrassment at work, obviously only dark heavy pants during the period, tucking my legs under me so that if I did have a bleed through it was onto my own pants, not the chair at work ( which did happen on a number of occasions).
I was prescribed Mefenamic acid and at tranexsmic acid at different points during this journey, I had tried hormonal birth control including an injection that made me bleed for months on end and an implant that I would latter need removed due to the continued bleeding whilst it was in place. I conceived two children on the oral contraceptive and this also caused me some other issues ( weight gain etc)
I saw 2 different specialists who both recommended a hysterectomy despite my being under 40. I found this extremely distressing.
My GP was away and I saw a different GP who looked at my file and noted that I had been taking an iron replacement for a number of years – I broke down in tears- , the GP did the iron test and found the iron was still low, when we discussed this she sent me for iron injections and an ultrasound. I now have staining on my buttock from the iron injection, it looks like a nasty bruise that I was told will stay for a number of years.
The ultrasound showed a “fibroid” so she referred me to another specialist. I was reluctant to go again as I didn’t want to be told I needed a hysterectomy again . I attended the joint clinic with gynaecologist and interventional radiologist. They listen to my story and looked at my ultrasound scan and suspected adenomyosis. They suggested me to have an MRI to confirm the diagnosis. In deed the MRI showed adenomyosis, and it was NOT fibroid. Finally someone has found the cause of my 15 years of suffering and offered UAE as an alternative to hysterectomy.
I had the UAE and my periods has never been so light before. I have to get rid of all my maternity pads and purchase normal pads. I was even swimming at my period time” KLB
How was adenomyosis diagnosed in the past and why was it neglected?
In the past when there was no means of accurate imaging to diagnosis adenomyosis, the diagnosis was only made after hysterectomy when the uterus was examined by pathologists. Up to 70% of hysterectomy specimen actually showed evidence of adenomyosis. Being a benign non-cancerous condition without effective specific treatments, there was no tenacity in making the correct diagnosis of adenomyosis. Without correct diagnosis, some futile, unnecessary and ineffective procedures might have been performed.
We believe early diagnosis is prudent in the management of adenomyosis, for women seeking fertility and symptom control. Effective treatments are now available. By raising awareness of this disease and applying the correct investigation pathway, early diagnosis can be achieved. Hysterectomy should no longer the only way to diagnosis and treat adenomyosis in the 21st century.
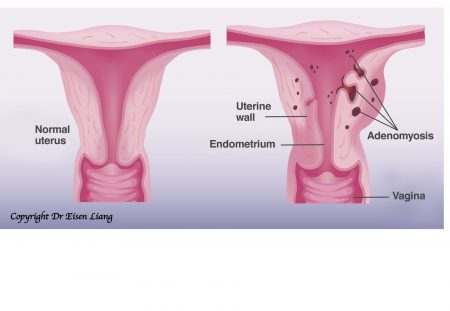
When a transvaginal ultrasound is done, much attention is paid to exclude nasty cancerous conditions in the ovaries or the cavity of the uterus. Any abnormalities of the ovaries like ovarian cysts are carefully documented. Any thickening of the lining of the uterus, polyps or growths within the uterine cavity are carefully examined. Any fibroids (benign tumours of the uterine wall) are measured and documented. By now, the sonographer has spent more than 20 minutes and pretty exhausted. Nasty tumours of the uterine wall (called sarcoma) are extremely rare, and they are usually large, just look like any fibroids that are very commonly seen, and ultrasound is not able to tell if they were sarcoma or not. There is the tendency to think all uterine muscle wall lesions are benign and non-cancerous, and therefore there is no tenacity to be absolutely correct in distinguishing fibroids from adenomyosis or picking up adenomyosis in what is almost normal looking uterus.
Adenomyosis has a wide range of manifestations. It can be very superficial and therefore ultrasound signs of adenomyosis can be very subtle. When adenomyosis is diffuse, there is no “focal” abnormalities to be seen on ultrasound, and only subtle changes in the texture if the uterine muscle layer is seen. When the adenomyosis is focal, it is often mistaken as fibroids. When fibroids are present, adenomyosis can be concealed.
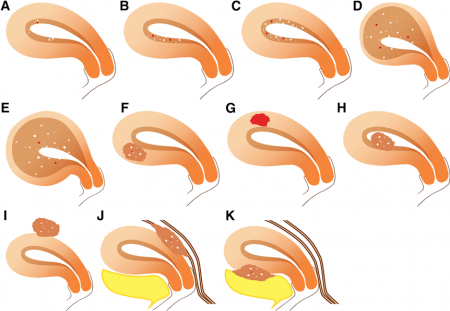
Classification of Adenomyosis
A, B, C: superficial adenomyosis. D and E: diffuse adenomyosis. F: intramural adenomyoma; G: cystic adenomyoma; H: submucosal adenomyoma; I: subserosal adenomyoma; J: posterior external adenomyosis; K: anterior external adenomyosis. Adopted from Basot et al .
There is limitation for ultrasound to accurately diagnose adenomyosis. Besides, missing the diagnosis of adenomyosis is not thought to be as bad, or as consequential as missing uterine cancer or ovarian cancer. Some might even think that adenomyosis wouldn’t kill, so what is the fuss about it?
As we have seen in Chapter 1, missing the diagnosis of adenomyosis means women are not getting an answer why they are having severe symptoms, and might have been put through futile, unnecessary and ineffective procedures and treatments, such as unnecessary laparoscopy, ineffective D&C procedure, inappropriate endometrial ablation, difficult / impossible attempted surgical removal. Of course, if we choose to stay in the last century, who cares what is in the uterus, just whip it out with a hysterectomy. Women of the 21st century deserves modern and individualised approach to their menstrual issues, and therefore making the diagnosis of adenomyosis is prudent to their optimal treatment.
In clinical practice, we know that MRI is far more accurate to diagnose adenomyosis, especially the superficial and diffuse adenomyosis with subtle signs on ultrasound. We also know that MRI can easily distinguish fibroids from adenomyosis. However, MRI is more expensive and do not attract a rebate by Medicare in Australia. Only staging of cervical cancer attract a rebate for MRI of women’s pelvis. If this is not gender inequality, I don’t know what else is.
More about diagnosing adenomyosis:
To make early diagnosis of adenomyosis, awareness of the disease and clinical suspicion is most important. Although heavy menstrual bleeding and period pain are rather common symptoms, the combination of these symptoms should raise suspicion.
To make early imaging diagnosis, we need to understand what we are looking for. Remember adenomyosis is due to the presence of endometrial tissue in the muscle layer of the uterus. Therefore, we look for the evidence of endometrium in the muscle layer. Endometrium is the lining of the uterine cavity and is the active layer with glands that changes throughout the menstrual cycle. The endometrial tissue is rich in cells, fluid and protein. When this tissue is entrapped within the uterine muscle wall, they can be seen as small cysts in the wall. Micro haemorrhage can occur within these entrapped areas of endometrium. When these cysts are microscopic, the wall simply looks “heterogeneous”. The uterine muscle cells react to this invasion of the endometrial tissue by enlargement and thickening. As a result, the uterus is often enlarged, with one wall thicker than the other.
Ultrasound is best performed using high definition transvaginal probe to see the details of the wall of the uterus. The uterus is often enlarged, and looks globular, more rounded and plumper. Normally the uterus is no more than 60mL in volume measurement, looks slender with a pear shape. The wall thickness can be asymmetrical, meaning the back wall is thicker than the front wall, or vice versa. The wall is often “hetereogeneous”, in other words, “it just doesn’t look normal”. There could be so called “Venetian blinds artefacts”, simply just exacerbation of the heterogeneous uterine muscle wall due to the presence of microcysts. Visualisation of cysts in the uterine muscle wall is highly indicative of adenomyosis, but this is not a common feature.
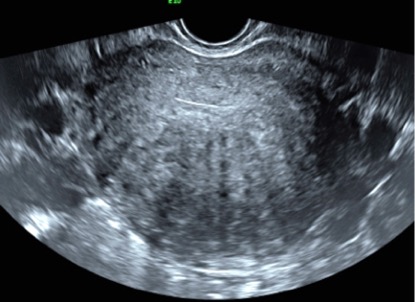
Figure 3a. Adenomyosis is seen as asymmetrical wall thickening, Venetian blinds artefacts and subtle small myometrial cysts. (Image courtesy of Dr Linda Atkins, UltrasoundCare)
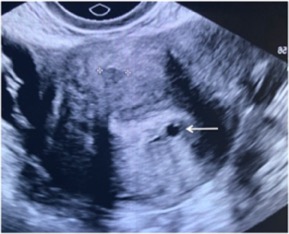
Figure 3b. Adenomyosis is seen as a globular shaped uterus with a myometrial cyst (arrow).
MRI can visualise exquisite details of the uterine wall with great clarity. MRI exhibits very good contrast between different soft tissues types. On MRI, endometrial tissue is bright, and normally is seen lining the cavity of the uterus. Invasion of this endometrial tissue into the muscle wall is easily spotted. Sometimes evidence of bleeding into these entrapped endometria within the wall of the uterus is observed. Typically there is also thickening of “junctional zone”, a inner layer of tightly packed uterine muscle cells. This layer is normally dark, and no more than 8 mm in thickness. When there is invasion of endometrium into this layer, together with reactive uterine muscle cell enlargement, the junctional zone (JZ) is thickened. JZ of 12 mm is said to be definitive for the diagnosis of adenomyosis on MRI and many adenomyosis researchers use this criteria. For small uterus, the absolute thickness is less meaningful and therefore the other accepted criteria are JZ more than 40% of total uterine wall thickness or the difference between the front and back wall of the uterus is more than 5mm.
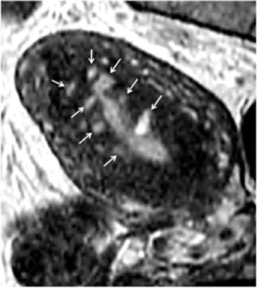
Figure 4a. Adenomyosis with multiple bright signal foci (ectopic endometrial tissue) within the thickened junctional zone (reactive myometrial hyperplasia).
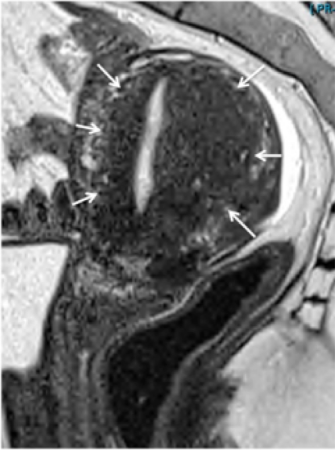
Figure 4b. Adenomyosis with junctional zone thickening of the back wall of the uterus.
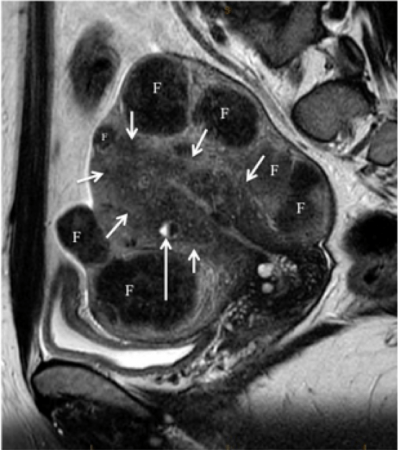
Figure 4c. Difference of adenomyosis and fibroids are clearly seen on this MRI. Adenomyosis is seen as irregular junctional zone thickening (short arrows) with a haemorrahgic cyst showing fluid-fluid level (long arrow). Coexisting fibroids are marked with “F”. Note fibroids are easily distinguished from adenomyosis on MRI.
Both ultrasound and MRI have been shown to be highly accurate in making the diagnosis of adenomyosis. Analysis of research studies has shown slightly higher pick up rate by MRI than ultrasound, and MRI is more often correct than ultrasound.
Ultrasound is more widely available and less expensive than MRI. However, ultrasound image is obtained with a hand held probe and is highly dependent on the skill and experience of the sonographer taking the pictures. Studies showing high pick up rate and accuracy are often from academic centres with special interest in adenomyosis. In real world practice, we have seen many cases missed by ultrasound. Ultrasound performed by imaging centres specialized in women’s health might have a higher pick up rate.
In our practice, we see fibroids and adenomyosis co-exist in about 50% of cases. Uterine fibroids quite often obscure ultrasound visualisation of adenomyosis. Focal adenomyosis was often mistaken as fibroid. Some women with severe symptoms might have adenomyosis in a small or normal sized uterus, where ultrasound signs are subtle or absent.
When adenomyosis is suspected in women with heavy and painful periods, this should be clearly indicated on the imaging request to alert the medical imaging specialists to look for these subtle signs.
CT scans are not useful for diagnosis of adenomyosis. CT scan might have been performed looking for other causes of unexplained abdominal pain.
Laparoscopy is the best diagnostic test for endometriosis, that is endometrial tissue outside of the uterus. This is an invasive investigation that require 3 key holes in the abdomen and therefore general anaesthetic. If adenomyosis is suspected due to heavy menstrual periods in addition to period pain, then non-invasive imaging like ultrasound or MRI looking into the cross-section of the uterine muscle wall is more appropriate. Endometriosis and adenomyosis often co-exist. Women with adenomyosis are likely to continue to have pain following surgical excision of endometriosis .
Hysteroscopy involves using a camera to look inside the cavity of the uterus. This is required for the investigation of abnormal uterine bleeding: bleeding that is not just heavy period, bleeding when not having a period, bleeding in between periods, bleeding after sex, bleeding after menopause and in women having high risks of developing endometrial cancer (caner of the inner lining of the uterus). Ultrasound might have shown thickening of the endometrium (then inner lining of the uterus) or presence of polyp or small fibroids in the cavity of the uterus. Biopsy of lining and removal of polyps and fibroids can be done with the aid of this camera. The camera and instruments are inserted through the vaginal and then the cervix. The cervix needs to be dilated and therefore this procedure needs to be done under general anaesthetic.