Fibroids Treatment Options
Your choice of fibroid treatment depends on the type and severity of your symptoms, as well as the size and location of your fibroids. At Sydney Fibroid Clinic, fibroid treatment is tailored to each woman’s needs based on her symptoms, fibroid size and location, and personal preferences. SFC specialises in applying uterine fibroid embolisation as a minimally invasive alternative to hysterectomy, and we often combine medical treatments, UFE, and adjunct minimally invasive surgical procedures to help women to avoid hysterectomy. There is often no single “best” treatment for everyone, and a detailed discussion with a specialist experienced in a combination of fibroid treatment options is important to fully understand the benefits, risks, recovery time, and long-term outcomes of each option, to work out the most suitable treatment for you.

Medical Therapy for Fibroids
Tranexamic acid, nonsteroidal anti-inflammatory drugs (NSAIDs), birth control pills, or progesterone agents may be used
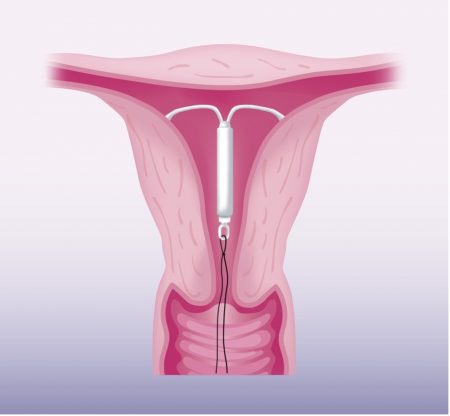
Mirena IUD for Fibroids
Mirena might reduce heavy bleeding but will not shrink fibroids. Mirena is an intrauterine device (IUD). It is a T-sh
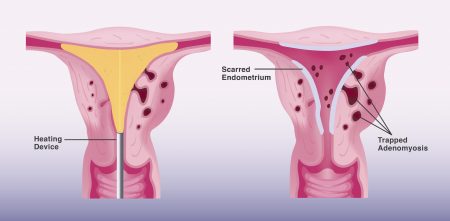
Endometrial Ablation for Fibroids
Endometrial ablation does NOT shrink fibroids themselves. Ablation uses heat energy to surgically destroy the inner l
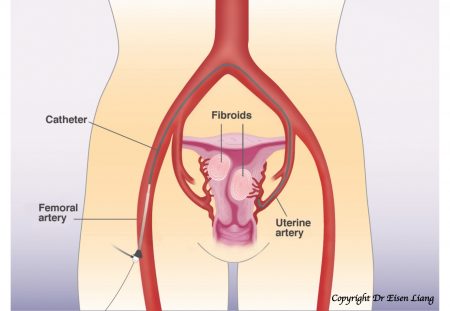
Uterine Fibroid Embolisation for Fibroids
Uterine fibroid embolisation (UFE) is also known as uterine artery embolisation (UAE). UFE is a safe, effective and m
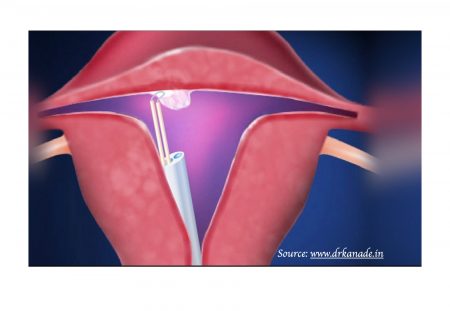
Hysteroscopic Resection for Fibroids
Hysteroscopic resection ( a guided curette procedure ) removes fibroids with the aid of a camera through the vagina and
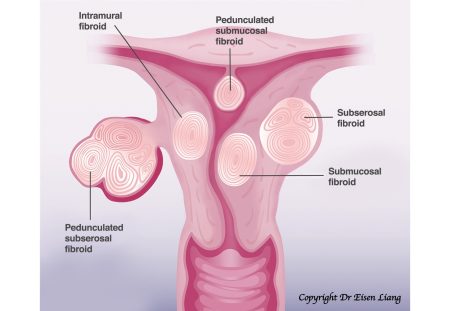
Myomectomy for Fibroids
A myomectomy is a surgical operation to remove one or a few fibroids. A myomectomy is offered to women who wish to retai