Adenomyosis Treatments
Watch the two Videos Below. At Sydney Fibroid Clinic, adenomyosis treatment is tailored to each woman’s needs based on her symptoms and personal preferences. SFC specialises in applying uterine artery embolisation as a minimally invasive alternative to hysterectomy, and we often combine medical treatments and UAE to help women to avoid hysterectomy. There is often no single “best” treatment for everyone, and a detailed discussion with a specialist experienced in a combination of adenomyosis treatment options is important to fully understand the benefits, risks, recovery time, and long-term outcomes of each option, to work out the most suitable treatment for you..
Treatment Option for Adenomyosis
Uterine Artery Embolization (UAE)

Medical Therapy for Adenomyosis
Medical therapy for adenomyosis refers to medications or pills aimed at easing symptoms. These treatments, however, are
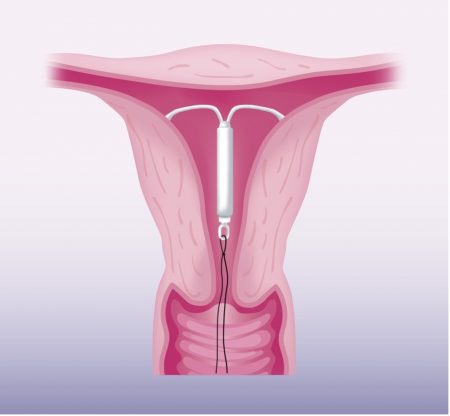
Mirena IUD for Adenomyosis
In A Nutshell Mirena is a progestogen-releasing contraceptive IUD. Mirena alleviates adenomyosis-related HMB and
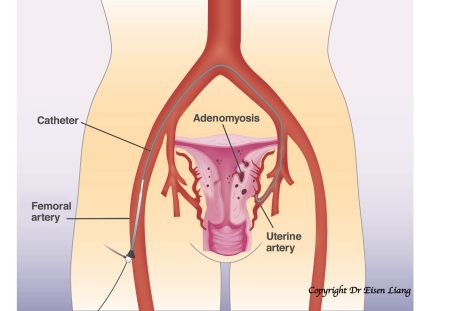
Uterine Artery Embolisation for Adenomyosis
UAE is potentially a life changing yet simple procedure for many women without resorting to hysterectomy. Uterine arter
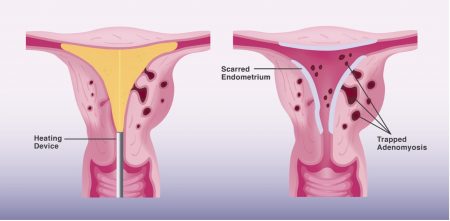
Endometrial Ablation for Adenomyosis
Endometrial ablation uses heat energy to destroy the inner lining of the uterus, so bleeding will be reduced. However
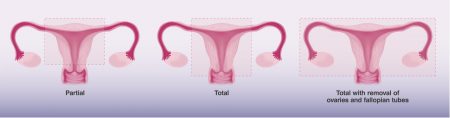
Hysterectomy for Adenomyosis
A hysterectomy is a surgical operation in which all or part of the uterus is removed. Hysterectomy is a major operati
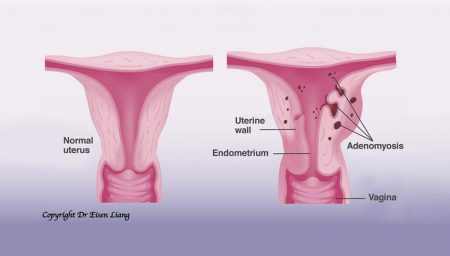
Surgical Removal of Adenomyosis
Generally speaking, adenomyosis is not suitable for surgical removal. Adenomyosis is often a diffuse infiltrative proces